Note: This article is in the process of being written
ACTIVITIES OF A HEALTH CARE FACILITY AND ITS MANAGEMENT
A health care facility provides services for the care of persons who are sick, the early detection of disease, prevention of health problems and promotion of wellness, as its core function. In order to offer these services, the healthcare facility needs to function as a business entity, a provider of hospitality services and a physical facility. In addition, strategic management is also important because the facility has to respond to changes in needs of its clients, technology, business environment, regulatory requirements and the welfare of its own staff. The management of activities, functions and services of a healthcare facility requires very complex organizational structures, policies and procedures.
Functions of a Healthcare Facility
CLINICAL FUNCTION AND ITS GOVERNANCE
The clients of a health care facility can be people who are sick (patients) or people who needs other services concerning their health. Nearly all clients of a hospital are patients. However, in a health clinic, many would be seeking services in relation to the prevention and early detection of disease as well as the promotion of wellness. They are mostly healthy.
CARE PROVISION AND CARE PROVIDERS
The term ‘healthcare’ is used to describe all services provided by health care facilities to its clients. These services or ‘care’ are delivered by care providers whose involvement can be direct or indirect. In a hospital the entire service is termed as ‘patient care’. Direct care activities refer to the set of well-defined (clinical) processes where care providers:
- interact face to face with clients/patients
- carry out procedures that affect them physically, physiologically or psychologically
Care givers providing direct care are called “clinicians”. By this definition they would include doctors, nurses, dietitians, therapists, clinical psychologists, counsellors and a few other professionals.
Clinicians are assisted and facilitated in their work by other professionals who, for the most part, do not come into direct contact with clients. They are referred to as “clinical support providers”. They perform tests, provide supplies and assist in the performance of other functions that have impact on the patient’s well-being. These Clinical Support Functions are listed below:
- Perform tests,
- Laboratory tests
- Imaging (Radiology) examinations
- Provide supplies
- Drugs (Pharmacy)
- Food and Beverage (Dietary Department)
- Blood (Blood Bank)
- Educational materials
- Sterile supplies
- Perform other non-clinical procedures
- administrative procedures (reception, registration, billing)
- set up/operate equipment and instruments
- manage clinical data (records)
However, the delineation of roles between direct and indirect providers is not very distinct because in some instances staff who traditionally provide clinical support also provides direct care. These include Dietitians, Clinical psychologists, Clinical Pharmacists, Clinical Microbiologists, Interventional Radiologists, Endoscopists, Optometrists, Audiologists, and many others. Also, personnel like radiographers (radiology technicians), whose job is to capture images, meet with patients and interact to a certain extent with them.
In the final analysis, the beneficial and harmful effects of care of the client are affected by both direct care (by clinicians) and indirect care (by clinical support providers). It is obvious that for health care to be successful all that participate in its delivery need to work together.
GOVERNANCE
Governance refers to all efforts that promote of the integration of various parts of an organisation to enable the accomplishment of common goals. This is accomplished using enablers consisting of a uniform set of cultural norms, ethical principles, means of interaction, policies and procedures. From a service delivery perspective, governance is different from operations management. Governance provides the general regulatory framework and the sociocultural environment necessary for facilitating the functions of the organization. It is applied to the entire organization. In a health care facility, the part that guides the business functions is termed as ‘Corporate Governance’ and that for clinical care is called ‘Clinical Governance’. The purpose of clinical governance is to create and maintain an environment that is conducive for achieving the goals of healthcare (refer http://iog.ca/defining-governance/ ).
Governance acts as the framework and creates the necessary environment. The actual execution of functions is managed through Operations management which is the more specific means of planning and controlling the realization of a particular service or a range of similar service products. It is performed by the facility manager (CEO) or heads of clinical departments (HOD) and units. In fact, in many instances the clinical care provider in charge is responsible for the operations management of the service delivery of his/her case.
Governance is only possible if the people involved are willing to adhere to uniform set of rules, ethical principles, policies and procedures by virtue of belonging to an organization or a regulated professional group. Otherwise, the achievement of common goals can only be attempted through advocacy. The promulgation and control of governance requires the assignment of authority and responsibility to certain individuals organized in a certain manner.
CLINICAL GOVERNANCE
It is generally agreed that clinicians and clinical teams have the prerogative and responsibility of managing persons under their care. Clinicians are generally customer/patient focused and have the welfare of their customer/patients at heart. However, a clinician does not and cannot operate on his/her own. The success of care delivery is dependent on proper input, processes and environment that are provided by the management. Complete care depends substantially on contributions by other clinicians, allied healthcare professionals and clinical support providers.
There is a need for many aspects of clinical patient care including the philosophy, goals, approaches, policies and practices to be streamlined in order to achieve the objectives of healthcare. This can come only through consensus. These areas of common interest relate not only to the practice of medicine but also include areas such as training, service delivery methods, information sharing and the optimization of the use of (usually scarce) resources. Clinicians as a group must be responsible for agreeing on standards plus monitoring and ensuring them. It is accepted that the Chief Executive officer or Director of the hospital is responsible for executing policies and ensuring that the hospital is functional. However, for the development of policies and procedures relating to clinical matters and their implementation, a management team made of representatives of all persons involved in care delivery is necessary.
In summary, Clinical governance refers to the advocacy, realization and assessment of:
- General regulatory framework and the sociocultural environment necessary to guide and facilitate clinical functions
- The set of rules, ethical principles, policies and procedures that guide service delivery
Clinical governance is applied to all clinical and clinical-support departments and units of the entire health care facility.
Governance and Operations Management
The definition Clinical governance used in this discussion is substantially different from that advocated by the National Health Service of United Kingdom (NHS) who defines it as “a systematic approach to maintaining and improving the quality of patient care within a health system”. (refer https://en.wikipedia.org/wiki/Clinical_governance ). The NHS definition narrows the scope by associating it with management of quality (and confining it further to seven elements) instead of covering the governance of all aspects of health care service delivery.
THE SCOPE OF CLINICAL GOVERNANCE
In a healthcare facility, the management of service delivery operations, business functions, upkeep of utilities and provision of hospitality services is the responsibility of the office of the Chief Executive Officer (CEO) or Hospital Director. This allows clinicians and clinical support providers to concentrate on clinical care. However, in many matters both at planning and execution level, the CEO need to be advised by the clinicians as a group.
Clinical Governance covers both the direct and indirect clinical care given to clients. The scope is further delimited by the type of services provided by the facility. The functions addressed by governance are those that apply throughout the organization. It is hoped that the sociocultural environment and the regulatory framework advocated prevail in all units and departments.
THE PURPOSE OF CLINICAL GOVERNANCE
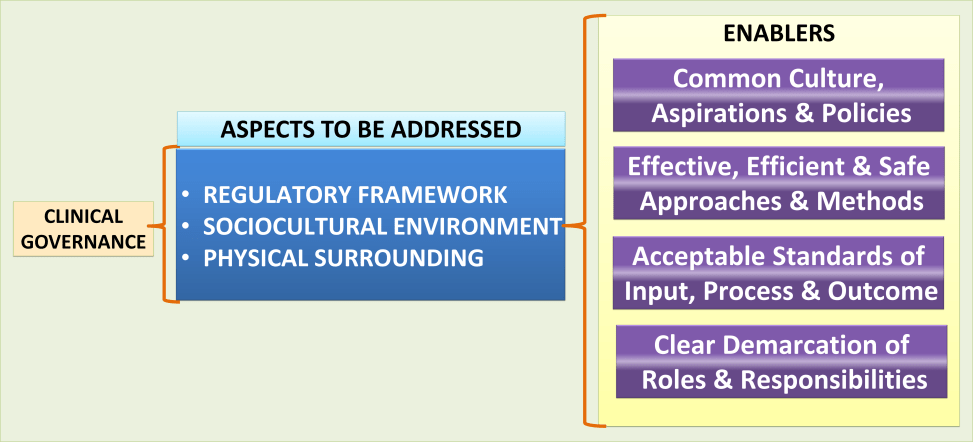
The processes of governance include advocacy, realization and control. The areas addressed by Clinical Governance include:
- Advocating belief in common philosophy, aspirations, culture and goals
- The use of approaches and methods approved by the health care profession
- The adherence to set norms and standards (of outcome and processes)
- Demarcation of roles and responsibilities (one’s own and that of others)
Conceptual Framework of Clinical Governance
COMMON PHILOSOPHY, CULTURE AND GOALS
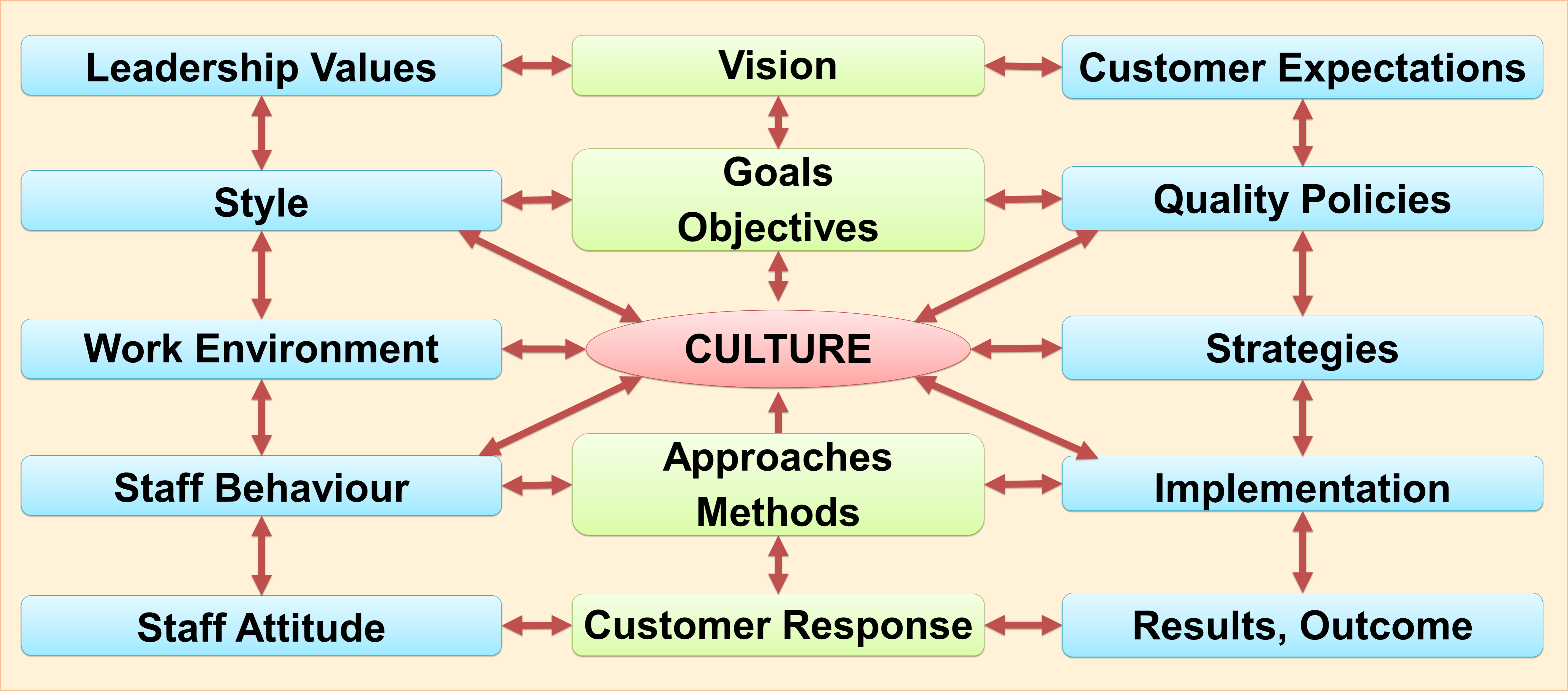
Common philosophy, culture and aspirations guide and bind the organization. They permeate all aspects of service delivery, determines how it is delivered and influences the behaviour of care providers. They are the overriding factors that decide approaches, methods and standards.
Values and aspirations shape culture. However, actual practices, attitudes and behaviour determines what customers perceive as the culture of the organization. These determining factors, in turn, are dependent on the physical and sociocultural environment as well the attributes of care providers as individuals and as a team/group.
The universal beliefs/values regarding healthcare are enunciated in the United Nations charter and the formal declarations of the professional bodies (e.g. code of conduct of medical council or associations). These need to be absorbed to form the basis of clinical governance. They include:
- equity
- respect for human dignity
- aspiring to provide the best care possible
- to do no harm
Care providers are inculcated with these beliefs during their professional training. In daily practice, they need to be guided by two main attributes
- professionalism
- ethical practice
Professionalism refers to practice of consistently using the special knowledge competence and values expected of a health care provider in daily practice for the benefit of the individual and community being served. The knowledge expected of a professional includes theoretical knowledge plus those absorbed through training and exposure. Care providers need to have the commitment to retain their knowledge and to expand it through life-long learning. Competence refers to technical, communication and reasoning skills. When performing procedures, the care provider need to exercise due care and diligence. He/she need to have the capability to choose and implement the most effective, appropriate and safe approaches, modalities and methods. (read more at https://drdollah.com/care-processes-overview/care-plans/ ). He/she should be aware of his/her own limitations and be ready to consult and refer persons under his/her care to others with the appropriate expertise including those outside of their own organization.
Credentialing of Healthcare Professionals
The healthcare facility must ensure that healthcare professionals it employs have adequate knowledge and skills plus possess the right attitude. This is done through the process of Credentialing i.e., a formalised procedure of assessing the credentials of each care provider before their employment. This is usually done by a sub-committee under the ambit of Clinical governance. The procedure includes:
- verification of their qualifications and experience
- assessing their attitude and moral standing
- determining the scope of practice (functional limits delineated by areas of expertise)
- assignment of duties and responsibilities (job description)
The Clinical Governance Committee advises by laying down policies and the facility’s management is responsible to follow through with it when vetting employees involved in patient care.
Ethics
Values refers to the internal beliefs, and attitudes consistent with being a care giver and is manifested as behaviour. Expected values include altruism, empathy, equity, honesty, and transparency. Respect for human dignity is paramount. All these values are laid out as professional ethical standards i.e., the standards of conduct required of a health care provider. Altruism translates into wishing for the best for those under their care and above all to do no harm. Honesty is translated into transparency and accountability which in turn requires the care provider to give appropriate information to enable the client to make informed decisions alleviate his/her worries. A proper provider-client relationship need to be maintained. Interventions are done only with the consent of the client.
Culture
The general goals of the organization need to be clarified and then translated into policies and objectives of every service it intends to deliver. Differences in approaches in service delivery can occur with the business model which can be:
- profit oriented
- not for profit
- charitable
However, these should be confined to policies and procedures regarding administrative functions and hospitality services. Business considerations should not affect the equity of clinical care or choice of approaches and methods.
MANDATING THE USE OF APPROVED POLICIES AND METHODS
Clinical care must necessarily be based on scientific medicine. It is important that approaches and methods are evidence-based i.e., scientifically proven and rely on sound principles. The evidence need not necessarily be proven by randomized controlled trials. Modalities, equipment and instruments must be chosen after careful technology assessment. Appropriateness and cost-effectiveness are also taken into consideration. The Clinical Governance Committee must guard against the choice of approaches, methods, or modalities for purpose of financial gain or prestige.
It is obvious that approaches and methods must be aligned with the organization’s philosophy, goals and policies including its business model. As such, standard operating procedures that are used commonly throughout the organization need to be uniform both in design (i.e., as documented) as well as in implementation.
Maintaining a Record of Care Given
An aspect of healthcare that should be taken seriously is the documentation of data regarding the care given and whatever else that transpires during the episode of care. There should be an effective means of disseminating these data among care providers. Proper records must also be kept for medico-legal requirements. To read further, please refer to article on medical record.
CONFORMANCE TO SET NORMS AND STANDARDS
Every country has its own laws and regulations regarding the conduct of healthcare service delivery. It is mandatory that policies procedures and standards of the healthcare facility conform with them. Also, standards set by the health care profession such as professional or accreditation bodies need to be taken into consideration.
The most important standard to be set is that relating to the outcome of care. Input and process standards will then be set so as to achieve the desired outcome. The role of clinical governance is to advocate general principles by which standards are set in terms of the criteria and the measurements to be used as well as the level expected. It is the duty and responsibility of departments, units and care providers (individually or as a team) to determine the standards for their service products.
The interrelationships of the input, process and outcome is described as the Systems Theory of Operational Management
The components of the operational management when applied to healthcare can be as depicted below:
Input Standards
Healthcare service delivery requires various input including
- The physical facility (rooms and spaces)
- Equipment, machines and instruments
- Raw material (drugs, sutures, dressings, chemicals etc.)
- Human resource (care providers)
- Information
As part of governance, the organization need to promote and ensure that all aspects of service delivery conform to accepted standards. Some of the standards regarding the physical facility can be at the discretion of the organization but those relating to safety and effectiveness are governed by strict laws. Utilities such as electricity, gas, water and steam must conform to exacting standards. Only machines approved by relevant authorities (e.g., Food and Drug Authority) should be used throughout the facility. They should be properly maintained so that they are functional and safe when used. All raw material especially drugs need to be procured from reliable sources and properly stored.
The health care facility must ensure that all care providers employed have the necessary knowledge, skills and attitude to perform duties assigned to them. The body in charge of clinical governance need to advice the CEO regarding the recognition of qualifications, verification of credentials and assessment of competence of clinical staff. It is also important to ensure that adequate numbers of relevant staff are available whenever a certain service is delivered. New staff must undergo proper orientation before being put on duty.
Data derived from operations and reference information are required by care providers in order to provide effective, efficient and save care. Information must be provided in a timely and adequate manner and in a format that is easily understood. The management should ensure accuracy, integrity, availability, security and confidentiality of these records. The desirable characteristics of the information system in healthcare is given in another article.
Process Standards
A substantial portion of the activities of the delivery of care must be conducted using similar processes, technology and materials throughout the organization. It is imperative that the most effective, efficient and safe way is determined and followed. This applies to all types of processes including technical, communications, cognitive processes, administrative and data management processes. Clinical governance has an important role to play in standardizing how the process is to be carried out, by whom, when, at what speed and the specifications of its output.
Relationship between Input, Process and Output
It is true that for each service product, the combination and sequence of the processes are usually different. Also, there may be processes unique to a particular service. There is a need, therefore, for standardized policies, work procedures, instructions (Standard Operating Procedure [SOP]) to be developed by the department, unit or individual care provider providing the service. Yet basic common processes need to be conducted in the manner recommended by the organization.
Outcome Standards
The quality features formed by characteristics of the environment, facilities, machines, staff attitude, staff behaviour and indeed the whole organizational culture contribute to the perception of quality. These features serve the secondary needs of the client. However, satisfying the primary needs of the client is undoubtedly the most important final outcome of a service. Therefore, the most important criterion for quality is whether the care given solves or alleviate the client’s health problems. The characteristics of the outcome of care should include:
- effectiveness (relative to the type and severity of illness)
- safety (avoidance of the harmful effects of treatment)
- appropriateness
- comprehensiveness
- continuity
While outcome is dependent on the type of illness, its severity and the health status of the client, the standards set, and the criteria used for measuring quality must take into consideration all the above characteristics. Hence, an important role of clinical governance is to inform, guide and assess departments, units, and individual providers the management of the quality of services provided.
Demarcation of Roles and Responsibilities
The smooth running of a health care facility depends on various components working in tandem. Hence, it is imperative that staff working in management, the clinical departments, and the support services know their roles and perform them diligently. Many care activities initiated by a care provider need to be continued through the efforts of many others before reaching its completion. The intermediate product of the initial provider becomes the input of the person performing the next process. It is important that a professional best suited for a job is assigned the responsibility. Certain staff (especially those in training or orientation) need to be supervised. Hence an important role of Clinical Governance is to oversee the activity of verifying credentials (credentialing) and assignment of privileges (privileging) of staff of the health care facility.
Effective and adequate communications is of major importance. Standard nomenclature, terminology and definitions need to be adopted. Mechanisms for discussion and consultation such as referral systems need to be agreed on. Above all, the means for documenting information and sharing them should be in place. Hence, Clinical Governance must involve itself in the design and operations of Clinical Information Systems and the Medical/Health Record.
As part of their professional ethics, care providers need to have respect for one another. Each must know his/her own area of responsibility that of other. While conflict should be avoided, Clinical Governance should be the means to promote their resolution if and when they occur.
IMPLEMENTATION OF CLINICAL GOVERNANCE
The implementation of Clinical governance is in stages encompassing:
- Formulation of scope, purpose and content
- Organization and Formalization
- Advocacy and Facilitation
- Operationalization
- Assessment and Review
MANDATE
Advocacy for clinical governance must originate from health care professionals.The Clinical Governance body by whatever name (e.g., committee, council) must be taken seriously and given an appropriate standing by both healthcare providers and the management. Its function is advisory and it should be consulted when decisions are to made regarding critical clinical matters. Yet, the mandate for the implementation of its resolutions must come from the management of the health care facility.
ORGANIZATION
Clinicians as a group need to be involved in the formulation, promotion and realization of common philosophy, goals, approaches, policies and practices relating to clinical practice. On the other hand, the execution of measures to put those in place need the authority that can come only from management (the CEO). Yet, it would be quite difficult for managers to impose rules on care providers considering that they are experts in their own fields and the demand for clinical independence. In some instances, the manager has to lean on the influence and moral authority of senior clinicians to put through various measures. Care providers especially specialists are likely to agree to rules and policies if they are consulted and be allowed to contribute in their development. Indeed cajoling, persuasion and negotiation is the more effective method.
Taking the above factors into consideration the formulation and promotion of various aspects of clinical governance are best done through Advisory Committees. On the other hand, their realization may require divestment of authority to the management (CEO or Director), Heads of Department or Executive Committees.
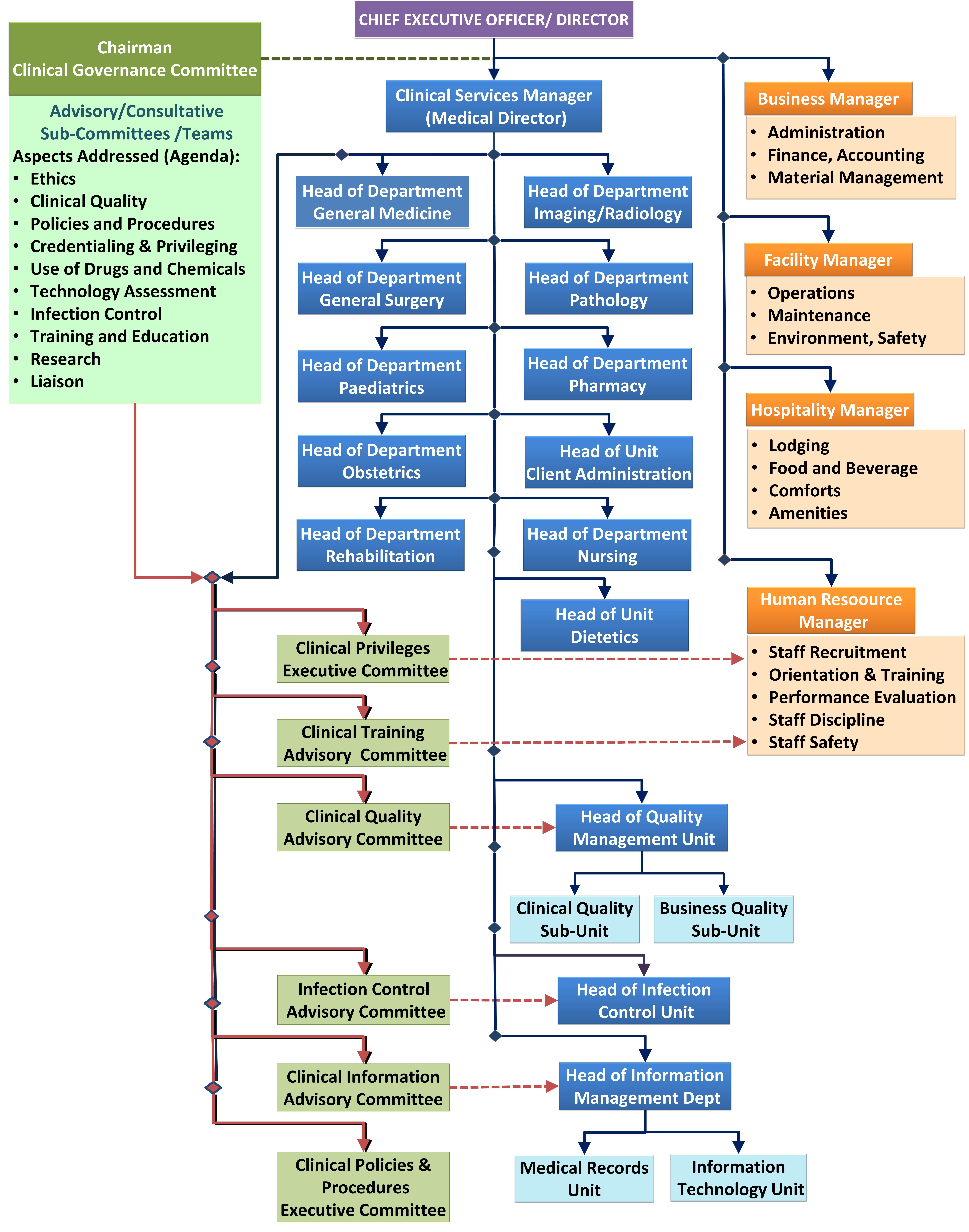
The main advisory committee may be called the Clinical Governance Committee. Currently, in most healthcare institutions the committee is called the Clinical/Medical Services Committee, the Medical Services Council, or Clinical Inter-department Conference (operationalized through meetings). Membership of the committee is made up of representatives from clinical and clinical support departments/units. It is customary, as a rule. for certain major departments to be included. Other departments or units are chosen to represent certain areas e.g. allied healthcare providers. Some membership may be limited to a certain term and be rotated. This umbrella committee is given the mandate to form other sub-committees to address various aspects of clinical governance. Members of sub-committees are usually co-opted. Clinicians involved in the main committee and the various sub-committees would have to contribute a considerable portion of their time to carry out these activities. therefore, it is expected that the committee would require a permanent well-equipped secretariat supported by a full complement of clerical staff. It is also expected that the Clinical Governance Committee does not involve itself in the actual operations of service delivery, except for some defined areas where it is given executive authority.
Example of the Organization of Clinical Governance and the Relationship with the Executive Arm of the Institution
Leadership
The Clinical Governance committee should assume the leadership role. The Chairman of the committee becomes the de facto chief of clinical services and need to be accorded the respect that he/she deserves. This position can be appointed by the CEO/Director or elected by department/unit representatives after being nominated.
Roles and Responsibilities of the Committee
The Clinical Governance Committee represents all healthcare providers within the institution. Besides addressing the needs of the care providers, the committee need to be the advocate for the rights of clients (primarily patients) and the community as a whole. It has the duty to formulate, promote and realize the common philosophy, goals, approaches, policies and practices relating to clinical practice.
Overall, the role of the committee is advisory. Yet in some instances, members of the committee acting on its behalf will be co-opted into executive committees with executive functions.
MECHANISMS AND ACTIVITIES
In the formulation of common approaches, goals and policies the main task of the committee is in obtaining consensus. This is best done by having experts or work groups develop and document the initial proposal. This is tabled at the main committee and discussed at length to allow various stakeholders to put in their input and defend their interests. When the consensus is achieved it should be disseminated.
Function of Executive Committees
Carrying out the initiatives of the committee are usually done through sub-committees. To give some actions the force of authority, executive committees should be made up of representatives of Clinical Governance and the management (the CEO). Terms and conditions of these committees need to be clearly specified. These sub-committees must also be aware that their decisions and actions are subject to legal scrutiny.
Like all committees, the main mechanism for carrying out its activities is through meetings. It is important that the meetings are carried out in properly structured manner. Minutes should be kept meticulously. Discussions should be free and what transpires need to be transparent to others stakeholders outside of the committee. To ensure decisions are based on comprehensive and balanced information, a lot of research through literature review and even studies need to be performed. Individuals or teams can be assigned to do this.
Training and Orientation
A sub-committee should be formed to design orientation and training programmes by identifying training needs of new and existing clinical staff. It has the duty to monitor and ensure that they are implemented. The actual programme should be carried out by a unit within the human resource department in collaboration with various clinical departments.
The Clinical Governance Committee should promote a culture of continuous learning and ensure that the environment for it is in place. Continuing education and professional development activities would be carried out through various sub-committees.
Clinical Policies and Procedures
An advisory sub-committee would be responsible to propagate a common approach to patient care based on rational scientific principles and ensure that these are followed in all clinical departments. Policies and Procedures for areas of common interest should be developed on the basis of good scientific evidence and consensus including use of Clinical Practice Guidelines, technology assessment methods, Benchmarking and research. Examples of such common areas include Control of Nosocomial Infection, Use of antibiotics, Referral system, Resuscitation, Admission and Discharge policies and procedures, Risk management, resource utilization etc. The committee shall also oversee the development of Policies and Procedures in all clinical units / disciplines and ensure that they faithfully follow the philosophy and approach advocated by the institution. The main objective is consistency of policies, procedures and processes especially in common areas.
Credentialing and Privileging
The committee has the responsibility and authority to put in place mechanisms for ensuring that all clinical personnel are suitably qualified for the tasks and positions assigned to them. Part of this authority is to define the credentials deemed acceptable for various job positions and to delineate clinical privileges awarded to each care provider. The recognition and vetting of credentials is tedious. The assignment of privileges impinge on the scope of care a provider can be involved in. Because of this the sub-committee on Credentialing and Privileging need to have executive powers and therefore need the involvement of the management.
Quality Management
The committee is responsible for ensuring that the infrastructure, input, processes and systems in the hospital are conducive for effective, safe, and efficient clinical patient care. This can be accomplished by ensuring conformance to Accreditation and Quality Management system standards. The committee has the responsibility and is empowered to achieve, and maintain this conformance to standards for all the clinical services.
Besides the Clinical Practice Guidelines mentioned above, the committee is responsible for setting outcome and process standards for the common areas in clinical patient care, monitoring them and ensuring the achievement to these standards. Where Quality management is carried out by a separate committee, the Clinical Governance Committee will be responsible for ensuring that the quality of clinical services is given the required attention.
A very effective way of measuring quality in healthcare is the use of Medical Audit and the monitoring of indicators. The Clinical Governance committee need to foster and educate clinical departments/units and individual clinicians to measure the outcome of their services and compare them with accepted standards. The committee can make it obligatory for their results to be submitted. Otherwise, they should be encouraged to publish or make them known in some form.
Supervision of Clinical Research
The committee is responsible for monitoring and ensuring that scientific and ethical considerations are given due attention by personnel undertaking research. This activity may be delegated to a sub-committee.
Culture and Ethics
The committee endeavors to formulate and instill various cultural traits and codes of ethical conduct among all clinical personnel.
Liaison Committees
Where resources are shared or the function of a section/department /unit is very dependent on the resources of another, the formation liaison committees are beneficial. Use of resources can be optimised and policies and procedures can be streamlined. The Operation Theatre/Services Committee is a good example. Committees that stimulate cooperation between clinical departments/units and clinical support services (laboratory, radiology and pharmacy) are necessary to standardize procedures and resolve conflicts.
Ensuring Regard for Roles and Responsibilities
Border management and settlement of disputes and grievances relating to clinical patient care requires the intervention of committees. Limits to interdepartmental roles and responsibilities need to set and respected. Some committees can be given powers to regulate, supervise and execute changes.
While the allocation and disbursement of resources is the responsibility of the CEO, the committee is obliged to monitor and influence decisions and practices with regards to utilization of resources especially human resources.
Advocacy
Clinical Committees should advocate for the patient by making policies and decisions that puts importance on the welfare of the patient above all other considerations. One way would be to create and advocate a client charter
The committees should also be concerned of the welfare of workers especially regarding their safety, professional development and social cohesion.






Hi.
I love this summary. Well elaborated for both practice and academics.
Mind sending a ms word/ pdf to my email?
Kind regards,
Dr. Peter Mulatya
LikeLike